The Comprehensive Wound and Lymphedema Center at GBMC
Offering the latest advancements and modalities in wound healing
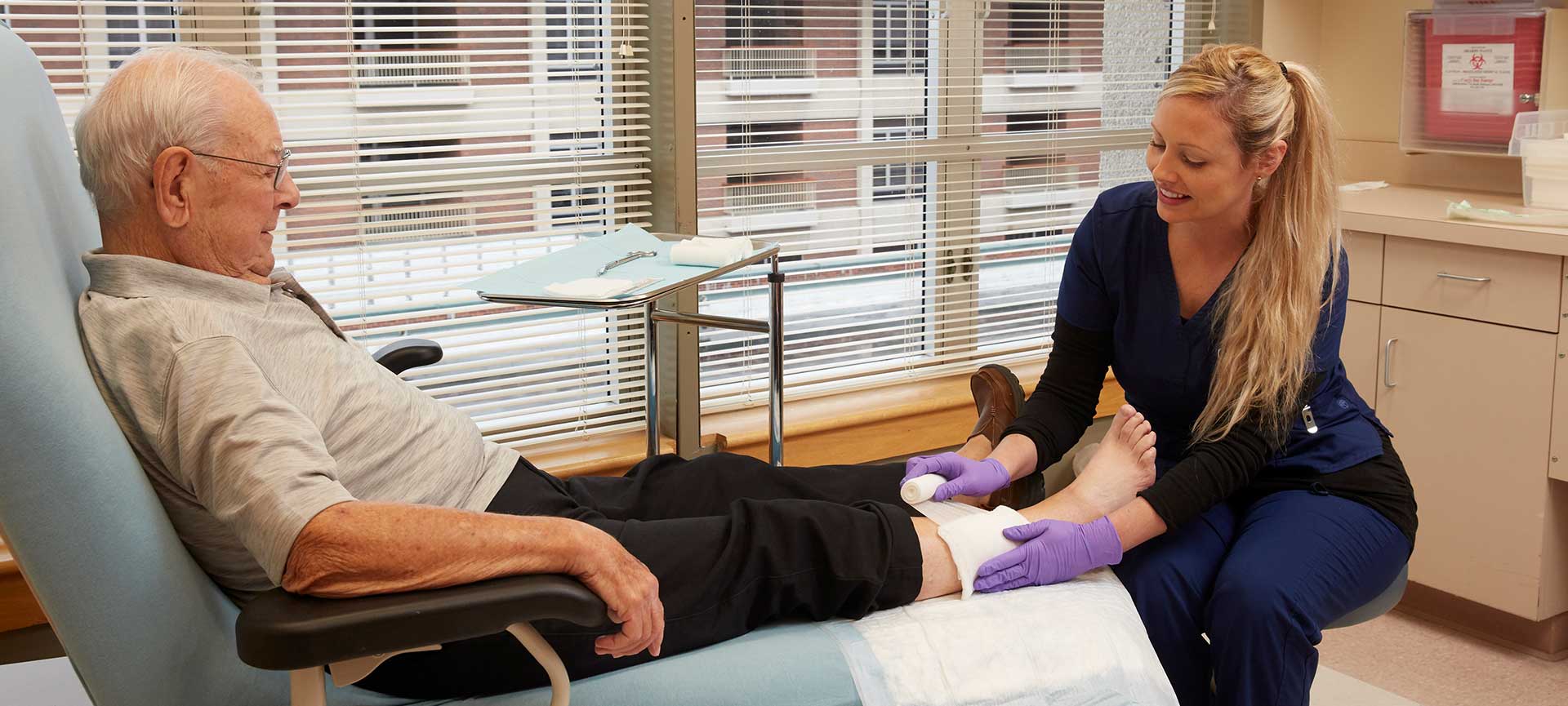
The Center utilizes the newest clinical tools in wound healing along with traditional clinical practices. We focus on the whole body throughout the healing process. This includes nutritional assessment and counseling, diabetic education, pain management, and patient and caregiver counseling.
Patients who benefit from hyperbaric oxygen therapy will receive a comprehensive evaluation to assess appropriateness of this therapy. They will be treated seamlessly in one of our five hyperbaric oxygen chambers following national guidelines.
Our Team

Jennifer A. Heller, MD, RPVI, FACS
Medical Director, Wound Center at GBMC; Director, Vein Center, Hyperbaric Medicine, Lymphedema, and Rehabilitation Medicine
Dr. Heller is the Medical Director of the Wound Center at GBMC. She is also Director of the Vein Center, Hyperbaric Medicine, Lymphedema, and Rehabilitation Medicine. She previously served as Assistant Professor of Surgery at Johns Hopkins University School of Medicine and as the founder and Director of the Johns Hopkins Vein Centers. A graduate of George Washington University School of Medicine in Washington, D.C., Dr. Heller completed her surgical residency, including a year as Administrative Chief Resident, at Boston University Medical Center. She completed her Vascular Surgery fellowship at New York Presbyterian Hospital.
Our Services
New Patient Information
When you come in, you will meet with our staff for a consultation, including an examination and medical history evaluation. Your wound care team will establish a treatment plan. Information regarding your progress will be submitted to your physician on an ongoing basis.
What you need to bring for your appointment:
- Any medical records
- Medication list and/or food allergies
- Insurance cards and forms
- If you require oxygen, please bring an adequate supply
- If you have diabetes, bring a snack and your medication
- Name, address, and telephone number of the physician(s) you currently see
- A legal guardian MUST accompany patients who are unable to comprehend or sign appropriate forms
- If you have an Advanced Directive, please bring a copy with you
- Reading material. Your first visit will last 1½ to 2 hours
Once you arrive:
One of our RNs and/or ancillary support staff members will introduce themselves, review your prior medical history, photograph, and measure your wound and provide you with additional information regarding the remainder of your visit. A provider specialty-trained in wound management will develop a plan of care with you.
Patient Testimonials
“The nurses, AP's, MDs etc. are all wonderful. Very competent and good teachers. I am impressed by how well procedures are conducted so appointments can be on the same day, whenever possible.”
“David Kitchen and the nurse were great. My wound is healing well because of them. Thank you!”
“I was seen at the wound clinic for my first time. The staff was wonderful. The nurse Mary Hoover made me feel comfortable and at ease. I was seen by Dr. Belgin. He explained why my foot had swollen and what caused the infection. He was able to trim away some callused area and referred me back to Podiatry for a follow up and new orthotics. I was able to wear a shoe for the first time in 3 months. Thank you, Wound Center!!”
“Everyone at this office (Wound Care) has been great with their services. Someone at the desk gave great directions of how to get to the Wound Center. The doctors and staff have all been great.”
“The care is wonderful. The nurses and other providers are caring, thoughtful, and excellent caregivers.”
“Such a caring and knowledgeable staff. Impressed that everyone spoke to my daughter who has disabilities and gave her time to respond. I feel more equipped about taking care of her wound.”
“The clinicians are efficient, practical, knowledgeable, and helpful.”
“So so grateful for all the nurses and especially Dr. Belgin for the wonderful care my husband has received since we've been coming here! It's been a long 3 years and they made it all worth it in the end. Thank you!!”
 Brian J. Belgin, DPM
Brian J. Belgin, DPM  Bradford Houck, PA-C
Bradford Houck, PA-C  David Kitchen, CRNP, CWSC
David Kitchen, CRNP, CWSC  Leora Schindelheim, PA
Leora Schindelheim, PA  Megan Tuffaha, BSN, RN, AGNP-C
Megan Tuffaha, BSN, RN, AGNP-C